Neural Repair After a Stroke: Bypassing the Blood-Brain Barrier with Intrathecal Stem Cells
Surviving a stroke is a life-altering event. Whether the stroke was ischemic, hemorrhagic, or a transient ischemic attack (TIA), the resulting damage to the brain can cause severe cognitive and physical impairments . Patients and their families are often desperate for recovery options, even years after the initial event .
Traditional rehabilitation primarily focuses on managing symptoms and relearning basic skills . However, at the Cellular Regeneration Clinic, we offer a proactive biological approach . Our advanced regenerative therapies aim to repair the actual neural damage left behind in the brain .
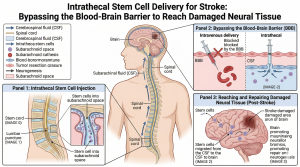

The Challenge of the Blood-Brain Barrier
The human brain is protected by a highly restrictive security system known as the Blood-Brain Barrier (BBB) . This semi-permeable membrane carefully filters your circulating blood . It is incredibly effective at keeping dangerous toxins and infections out of your central nervous system .
Unfortunately, this barrier also prevents most regenerative therapies from reaching the brain . Because stem cells are relatively large biological molecules, the BBB blocks them from entering if they are simply administered through a standard intravenous (IV) drip . To achieve true neural repair, we must utilize a specialized delivery method .
The Medical Necessity of Intrathecal Administration
To successfully bypass the Blood-Brain Barrier, our medical team utilizes a highly precise technique known as Intrathecal Administration . This procedure places the regenerative cells directly into your spinal canal . The spinal fluid then effortlessly carries the cells around the brain, allowing them to penetrate and begin repairing the damaged neural tissue .
This specialized administration requires absolute clinical precision . Therefore, a board-certified Anesthesiologist always performs this procedure at our clinic . Using a carefully guided lumbar puncture, the doctor safely introduces the cells into the spinal fluid . The process is fast, utilizes a local anesthetic, and is performed in a completely sterile clinical operating room .
Repairing Neural Tissue and Blood Vessels
Once inside the brain, Mesenchymal Stem Cells have been shown to target the damaged areas . The primary purpose of this therapy is to help repair and regenerate damaged neural and myelin sheath tissue . Furthermore, in the case of a hemorrhagic stroke, the cells actively support the repair of the severe blood vessel damage that caused the event .
Silencing Severe Neuroinflammation
A major obstacle to stroke recovery is chronic neuroinflammation . Following a stroke, the brain remains highly inflamed, which causes immense physical pressure on the surviving neural pathways . Stem cells act as powerful anti-inflammatory agents .
By significantly reducing this inflammation, the cells prepare the damaged areas for active regeneration . Additionally, stem cells possess the unique ability to replicate themselves within the spinal fluid . Consequently, this replication creates more exosomes over time, setting off a longer-term healing cascade that protects the brain .
The Importance of Systemic IV Support
While the intrathecal injection specifically targets the brain, a stroke deeply affects your entire central and peripheral nervous system . For this reason, a comprehensive stroke protocol also includes a high-dose Intravenous (IV) infusion .
The blood carries these IV stem cells throughout the body to repair potential nerve damage in your arms, legs, and gut . Furthermore, a stroke forces your secondary organs to work much harder . The systemic IV therapy can help repair this collateral organ strain . Patients looking to understand how systemic IV therapy supports overall vascular health can review our dedicated guide on stem cell heart therapy.
Premium Care and Advanced Laboratory Standards
Recovering from a stroke requires potent, highly viable cells . Extracting exhausted cells from a patient’s own body simply cannot provide the necessary biological energy .
Therefore, we exclusively utilize our in-house laboratory to cultivate ethically sourced, young Umbilical Cord Stem Cells . We maintain absolute control over the cellular quality, ensuring a viability rate of 99.99% for every patient . We encourage you to read our frequently asked questions to learn more about the safety and purity of our protocols.
By utilizing world-class clinic facilities, we provide stroke survivors with a safe and highly advanced environment to pursue their recovery goals .
Regenerative Medicine Specialist
Dr. Cota is a leading specialist in Regenerative Medicine and clinical Stem Cell application at the Cellular Regeneration Clinic He holds an ISSCA Certification and is currently completing his Master’s degree in Regenerative Medicine [27].
*Disclaimer: No positive outcome of any medical treatment is promised or implied. More than one round of treatment may be required. All sales are final with no refunds regardless of patient outcome. Results may vary between patients, as with all medical treatments there is no guarantee of any particular outcome. Please consult with our medical team to see if you are a candidate [28, 29].


